Emergence of polymyxin B as a viable treatment option in comparision to newer antimicrobials in Intensive Care Units: A study in North India
Keywords:
Resistance, ICU, Polymyxin B, Tigecycline, Floroquinolones, Carbapenem
Abstract
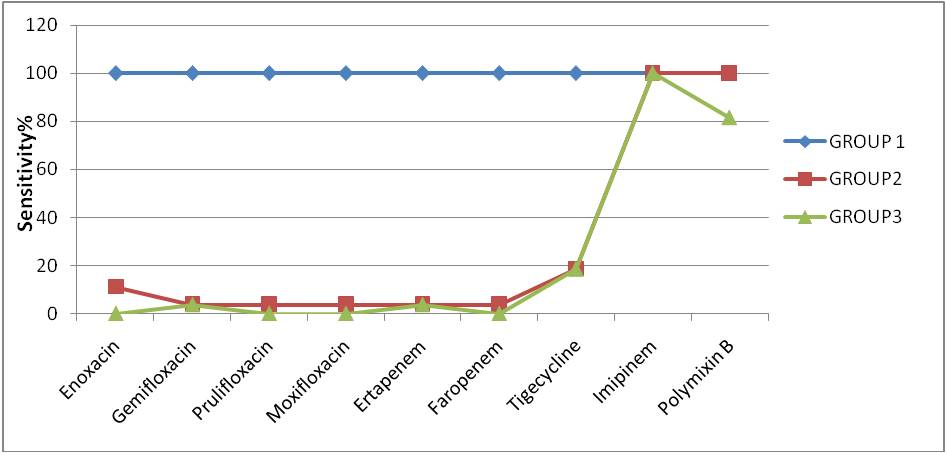
Background: Multidrug resistance (MDR) among gram-negative bacilli has increased substantially limiting the choice of antimicrobials. This study was conducted with the objective to determine the efficacy of tigecycline , polymyxin B, newer floroquinolones and newer carbapenems against MDR gram negative isolates.Methods: 90 clinical samples were obtained from ICU patients. On basis of antibiotic susceptibility to first line antibiotics isolates were divided into 3 groups- a)sensitive to all the first line drugs, b) sensitive only to injectables and c) resistant to all antibiotics except imipenem.These groups were then tested against enoxacin(10 μg), gemifloxacin (5μg), moxifloxacin (5μg), prulifloxacin (5μg), ertapenem (10μg), faropenem (5μg), tigecycline (15μg) and polymyxin B (300 units). Isolates were screened for ESBL, AmpC, CRE and MBL.Results: All the isolates in group 1 were uniformly sensitive to all the new antimicrobials tested. In group 2 susceptibility profile was as follows -100% sensitive to polymyxin B, 16.6% to tigecycline, 10% to enoxacin, 3.3% to gemifloxacin, moxifloxacin, prulifloxacin, ertapenem and faropenem. In group 3, 81.5% of the isolates were sensitive to polymyxin B, 13.2% to tigecycline, 3.3% each to gemifloxacin and ertapenem.. Isolates of the three groups were uniformly sensitive to imipenem(100%). 2(6.67%) of the isolates were ESBL producers and 30 (33.3%) were AmpC producers. No CRE and MBL were detected.Conclusion: Polymyxin B emerged as most effective antimicrobial in group 2 and group 3 with 100% and 81.5% sensitivity respectively. Use of polymyxin B will prevent injudicious use of imipenem and will decrease escalation of MBLs in our facility.References
1) Nordmann P, Cuzon G, Naas T. The real threat of Klebsiella pneumonia carbapenemase producing bacteria. Lancet Infect. Dis. 2009;9:228– 236.
2) Lautenbach E, Patel JB, Bilker WB, Edelstein PH, Fishman NO. Extended- spectrum b-lactamase-producing Escherichia coli and Klebsiella pneumoniae: risk factors for infection and impact of resistance on outcomes. Clin Infect Dis 2001; 32:1162–1171.
3) Reinert RR, Low DE , Rossi F, Zhang X, Wattal C, Dowzicky MJ. Antimicrobial susceptibility among organisms from the Asia/Pacific Rim, Europe and Latin and North America collected as part of TEST and the invitro activity of tigecycline. J Antimicrob Chemother 2007;60: 1018-1029.
4) Rizvi M, Khan F, Shukla I, Malik A, Shaheen. Rising Prevalence of Antimicrobial Resistance in UTI During Pregnancy: Necessity for Exploring Newer Treatment Options. Journal of Laboratory Physicians 2011;3:98-103.
5) Pramod MS, Robin DI. Ertapenem, the first of a new group of carbapenems. J. Antimicrob. Chemother. 2003; 52: 538-542.
6) Shin YM, Oh YM, Kim MN, Shim TS, Lim CM. Usefulness of Quantitative Endotracheal Aspirate Cultures in Intensive Care Unit Patients with Suspected Pneumonia. Korean Med Sci 2011; 26: 865-869.
7) Collee JG, Fraser AG, Marmion BP, Simmons A. Mackey and McCartney practical Medical Microbiology. In: Collee JG, Miles RS, Watt B, ed: Tests for the identifi cation of Bacteria. 14th ed. New Delhi, India: Elsevier, 2006:131-149.
8) Clinical and Laboratory Standards Institute 2014.. Performance standards for antimicrobial susceptibility testing: twenty fourth informational supplement: Approved standards M100-S24. Clinical and Laboratory Standards Institute, Baltimore, USA. 2014.
9) Lee KY, Chong HB, Shin YA, Yong KD, Yum JH. Modified Hodge test and EDTA disc synergy tests to screen metallo beta lactamase producing strains of Pseudomonas and Acinetobacter species. Clin Microbiol Infect 2001; 7:88-91.
10) Singh RK, Pal NK, Banerjee M, Sarkar S, Gupta MS. Surveillance on extended spectrum β lactamase and ampc β lactamase producing gram negative isolates from nosocomial infections Archives of Clinical Microb. 2012,3:1-7.
11) Grover N, Sahni AK, Bhattacharya S. Therapeutic challenges of ESBLS and AmpC beta-lactamase producers in a tertiary care center. Med. J armed forces, India, 2013;69: 4 -1 0.
12) Singhal S, Mathur T, Khan S, Upadhayay DJ, Chugh S. Evaluation of methods for Amp C β lactamase in gram negative clinical isolates from tertiary care hospitals. Indian J of Med. Microb. 2005;3:120-124.
13) Castanheira M, Sader HS, Deshpande LM, Fritsche TR, Jones RN. Antimicrobial activities of tigecycline and other broad-spectrum antimicrobials tested against serine carbapenemase and metallo-b-lactamase-producing Enterobacteriaceae: report from the SENTRY Antimicrobial Surveillance Program. Antimicrob Agents Chemother 2008;52:570–573.
14) Argyris M, Matthew EF. Colistin and Polymyxin B in Critical Care. Crit Care Clinics 2008;24(2):377–391.
15) Sekar M, Sekar U. Tigecycline Against Gram Positive and Gram Negative Isolates in a Tertiary Care Hospital .J of Clin and Diagnos Research, 2011;5(8): 1559-1563.
16) Behera B, Das A, Mathur P, Kapil A, Gadepalli R, Dhawan B. Tigecycline susceptibility report from an Indian tertiary care hospital. Indian J Med Res 2009;129:446-450.
17) Manoharan A, Chatterjee S, Madhan S, Mathai D. Evaluation of tigecycline activity in clinical isolates among Indian medical centers..Indian J Pathol Microbiol 2010;53 (4):734-737.
18) Livermore DM, Oakton KJ, Michael W C, Warner M. Activity of Ertapenem (MK-0826) versus Enterobacteriaceae with Potent β Lactamases. Antimicrobial agents and chemother. 2001;45:2831–2837.
19) Lee NY, Lee CC, Huang WH, Tsui KC, Hsueh PR, Ko WC. Carbapenem therapy for bacteremia due to extended-spectrum-β-lactamase-producing Escherichia coli or Klebsiella pneumoniae: implications of ertapenem susceptibility.Antimicrob Agents Chemother. 2012 ;56:2888-2893.
20) Mushtaq S, Hope R, Warner M, David M. Livermore Activity of faropenem against cephalosporin-resistant Enterobacteriaceae. Journal of Antimicrobial Chemotherapy 2007; 59:1025–1030.
21) Livermore DM, Mushtaq S, Nguyen T, Warner M. Strategies to overcome extended-spectrum β-lactamases (ESBLs) and AmpC β-lactamases in shigellae. Int J Antimicrob Agents, 2011;37(5):405-409.
2) Lautenbach E, Patel JB, Bilker WB, Edelstein PH, Fishman NO. Extended- spectrum b-lactamase-producing Escherichia coli and Klebsiella pneumoniae: risk factors for infection and impact of resistance on outcomes. Clin Infect Dis 2001; 32:1162–1171.
3) Reinert RR, Low DE , Rossi F, Zhang X, Wattal C, Dowzicky MJ. Antimicrobial susceptibility among organisms from the Asia/Pacific Rim, Europe and Latin and North America collected as part of TEST and the invitro activity of tigecycline. J Antimicrob Chemother 2007;60: 1018-1029.
4) Rizvi M, Khan F, Shukla I, Malik A, Shaheen. Rising Prevalence of Antimicrobial Resistance in UTI During Pregnancy: Necessity for Exploring Newer Treatment Options. Journal of Laboratory Physicians 2011;3:98-103.
5) Pramod MS, Robin DI. Ertapenem, the first of a new group of carbapenems. J. Antimicrob. Chemother. 2003; 52: 538-542.
6) Shin YM, Oh YM, Kim MN, Shim TS, Lim CM. Usefulness of Quantitative Endotracheal Aspirate Cultures in Intensive Care Unit Patients with Suspected Pneumonia. Korean Med Sci 2011; 26: 865-869.
7) Collee JG, Fraser AG, Marmion BP, Simmons A. Mackey and McCartney practical Medical Microbiology. In: Collee JG, Miles RS, Watt B, ed: Tests for the identifi cation of Bacteria. 14th ed. New Delhi, India: Elsevier, 2006:131-149.
8) Clinical and Laboratory Standards Institute 2014.. Performance standards for antimicrobial susceptibility testing: twenty fourth informational supplement: Approved standards M100-S24. Clinical and Laboratory Standards Institute, Baltimore, USA. 2014.
9) Lee KY, Chong HB, Shin YA, Yong KD, Yum JH. Modified Hodge test and EDTA disc synergy tests to screen metallo beta lactamase producing strains of Pseudomonas and Acinetobacter species. Clin Microbiol Infect 2001; 7:88-91.
10) Singh RK, Pal NK, Banerjee M, Sarkar S, Gupta MS. Surveillance on extended spectrum β lactamase and ampc β lactamase producing gram negative isolates from nosocomial infections Archives of Clinical Microb. 2012,3:1-7.
11) Grover N, Sahni AK, Bhattacharya S. Therapeutic challenges of ESBLS and AmpC beta-lactamase producers in a tertiary care center. Med. J armed forces, India, 2013;69: 4 -1 0.
12) Singhal S, Mathur T, Khan S, Upadhayay DJ, Chugh S. Evaluation of methods for Amp C β lactamase in gram negative clinical isolates from tertiary care hospitals. Indian J of Med. Microb. 2005;3:120-124.
13) Castanheira M, Sader HS, Deshpande LM, Fritsche TR, Jones RN. Antimicrobial activities of tigecycline and other broad-spectrum antimicrobials tested against serine carbapenemase and metallo-b-lactamase-producing Enterobacteriaceae: report from the SENTRY Antimicrobial Surveillance Program. Antimicrob Agents Chemother 2008;52:570–573.
14) Argyris M, Matthew EF. Colistin and Polymyxin B in Critical Care. Crit Care Clinics 2008;24(2):377–391.
15) Sekar M, Sekar U. Tigecycline Against Gram Positive and Gram Negative Isolates in a Tertiary Care Hospital .J of Clin and Diagnos Research, 2011;5(8): 1559-1563.
16) Behera B, Das A, Mathur P, Kapil A, Gadepalli R, Dhawan B. Tigecycline susceptibility report from an Indian tertiary care hospital. Indian J Med Res 2009;129:446-450.
17) Manoharan A, Chatterjee S, Madhan S, Mathai D. Evaluation of tigecycline activity in clinical isolates among Indian medical centers..Indian J Pathol Microbiol 2010;53 (4):734-737.
18) Livermore DM, Oakton KJ, Michael W C, Warner M. Activity of Ertapenem (MK-0826) versus Enterobacteriaceae with Potent β Lactamases. Antimicrobial agents and chemother. 2001;45:2831–2837.
19) Lee NY, Lee CC, Huang WH, Tsui KC, Hsueh PR, Ko WC. Carbapenem therapy for bacteremia due to extended-spectrum-β-lactamase-producing Escherichia coli or Klebsiella pneumoniae: implications of ertapenem susceptibility.Antimicrob Agents Chemother. 2012 ;56:2888-2893.
20) Mushtaq S, Hope R, Warner M, David M. Livermore Activity of faropenem against cephalosporin-resistant Enterobacteriaceae. Journal of Antimicrobial Chemotherapy 2007; 59:1025–1030.
21) Livermore DM, Mushtaq S, Nguyen T, Warner M. Strategies to overcome extended-spectrum β-lactamases (ESBLs) and AmpC β-lactamases in shigellae. Int J Antimicrob Agents, 2011;37(5):405-409.
Published
26-10-2015
Issue
Section
Original Article
Authors who publish with this journal agree to the following terms:
- Authors retain copyright and grant the journal right of first publication with the work simultaneously licensed under a Creative Commons Attribution License that allows others to share the work with an acknowledgement of the work's authorship and initial publication in this journal.
- Authors are able to enter into separate, additional contractual arrangements for the non-exclusive distribution of the journal's published version of the work (e.g., post it to an institutional repository or publish it in a book), with an acknowledgement of its initial publication in this journal.
- Authors are permitted and encouraged to post their work online (e.g., in institutional repositories or on their website) prior to and during the submission process, as it can lead to productive exchanges, as well as earlier and greater citation of published work (See The Effect of Open Access at http://opcit.eprints.org/oacitation-biblio.html).




